STD
Sexually transmitted infections (STI), also referred to as sexually transmitted diseases (STD) and venereal diseases (VD), are infections that are commonly spread by sexual activity, especially vaginal intercourse, anal sex and oral sex. Many times STIs initially do not cause symptoms. This results in a greater risk of passing the disease on to others. Symptoms and signs of disease may include vaginal discharge, penile discharge, ulcers on or around the genitals, and pelvic pain. STIs can be transmitted to an infant before or during childbirth and may result in poor outcomes for the baby. Some STIs may cause problems with the ability to get pregnant.
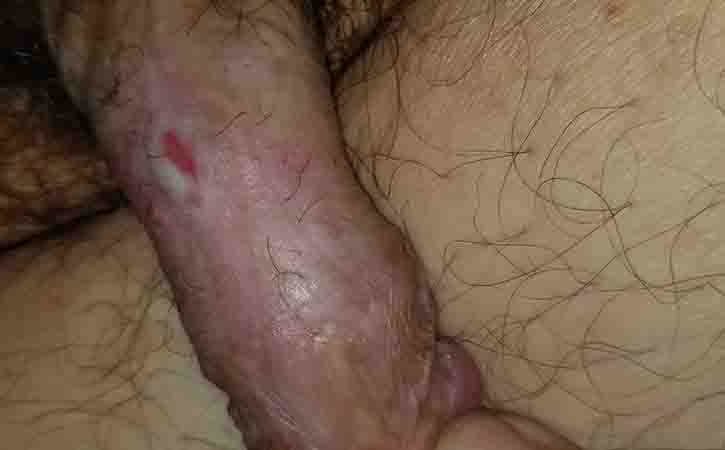
Syphilis (the Great pox) also known as lues, is an infectious venereal disease caused by the delicate spirochaetal micro-organism Treponema pallidum. The only known host is the human. It is increasing in incidence and is a great mimic. Syphilis is transmissible by sexual contact with infectious lesions, from mother to fetus in uterous, via blood product transfusion, and occasionally through breaks in the skin that come into contact with infectious lesions. If untreated, it progresses through 4 stages: primary, secondary, latent, and tertiary.
Syphilis that remains untreated for a long time can cause major damage to important organs, like the heart and brain. Without treatment, it can lead to disability, and death.
Characteristically, the incubation period is 9–90 days and the first sign is the appearance of the chancre (firm ulcer) at the site of inoculation, usually on the glans penis, prepuce or, less often, on the shaft in men and on the vulva in women. In homosexuals the chancre (firm ulcer) appears around or in the anus. The chancre (firm ulcer) is of variable size (0.5–3 cm in diameter) and has a sloughy and markedly indurated base. Untreated, it heals after 3–8 weeks. The four stages of syphilis are:
- primary
- secondary
- latent
- tertiary
Primary symptoms
One or many painless, firm, and round syphilitic sores called chancres (firm ulcer) are appear. These appear about 18-21 days after exposure.
Chancres (firm ulcer) disappear within 1-4 months, but, without treatment, the disease may progress to the next phase.
In primary syphilis stage also developed regional lymphadenopathy.
Secondary symptoms
Secondary syphilis symptoms include:
- a non-itchy rash/disseminated erythematous rash that is followed by a papulosquamous eruption, that starts on the trunk and spreads to the entire body, including the palms of the hands and soles of the feet and mucous membranes. It may be rough, red, or reddish-brown in color
- Oral(small clustered mouth ulcers), anal, and genital wart-like sores
- muscle aches
- fever
- sire throat
- swollen lymph nodes
- patchy hair loss
- headaches
- weight loss
- fatigue
These symptoms can resolve a few weeks after they appear, or they can return several times over a longer period.
Untreated, secondary syphilis can progress to the latent and late stages.
Latent syphilis
The latent phase can last several years. During this time the body will harbor the disease without symptoms.
After this, tertiary syphilis may develop, or the symptoms may never come back. However, the T. pallidum bacteria remain dormant in the body, and there is always a risk of recurrence.
Late or tertiary syphilis
Tertiary syphilis can occur 10 to 30 years after onset of the infection, normally after a period of latency, where there are no symptoms.
Symptoms include:
- damage to the heart, blood vessels, liver, bones, and joints
- gummas, or soft tissue swellings that occur anywhere on the body
Organ damage means that tertiary syphilis can often be fatal.
Neurosyphilis
Neurosyphilis is a condition where the bacteria have spread to the nervous system. It is often associated with latent and tertiary syphilis, but it can appear at any time after the primary stage.
It may be asymptomatic for a long time, or it can appear gradually.
Symptoms include:
- dementia or altered mental status
- abnormal gait
- numbness in the extremities
- problems with concentration
- confusion
- headache or seizures
- vision problems or vision loss
- weakness
Congenital syphilis
Congenital syphilis is severe and frequently life-threatening. Infection can transfer from a mother to her fetus through the placenta, and also during the birth process.
Without screening and treatment, around 70 percent of women with syphilis will have an adverse outcome in pregnancy.
Adverse outcomes include early fetal death, preterm or low birth weight, neonatal deaths, and infection in infants.
Symptoms in newborns include:
- saddle nose, in which the bridge of the nose is missing
- fever
- difficulty gaining weight
- a rash of the genitals, anus, and mouth
- small blisters on the hands and feet that change to a copper-colored rash and spread to the face, which can be bumpy or flat
- watery nasal fluid
Older infants and young children may experience:
- Hutchinson teeth, or abnormal, peg-shaped teeth
- bone pain
- vision loss
- hearing loss
- joint swelling
- saber shins, a bone problem in the lower legs
- scarring of the skin around the genitals, anus, and mouth
- gray patches around the outer vagina and anus
Infection with the causative organism, Treponema pallidum, may be congenital, acquired through transfusion with contaminated blood, or by accidental inoculation. The most important route, however, is through sexual contact (during oral, anal, or vaginal sexual activity) with an infected partner. Rarely, it can be passed on through kissing.
It can’t be transmitted by sharing a toilet with another person, wearing another person’s clothing, or using another person’s eating utensils.
It can also be passed from mother to a fetus during pregnancy, or to an infant during delivery. This is called congenital syphilis.
Antibiotic Therapy: Penicillin
Penicillin was established as an effective treatment for syphilis. Penicillin is the preferred drug for treating all stages of syphilis. Penicillin is the only recommended therapy for neurosyphilis, congenital syphilis, or syphilis during pregnancy. Rarely, T pallidum has been found to persist following adequate penicillin therapy; however, there is no indication that the organism has acquired resistance to penicillin.
The following regimens are recommended for penicillin treatment:
- Primary or secondary syphilis – Benzathine penicillin G 2.4 million units intramuscularly (IM) in a single dose
- Early latent syphilis – Benzathine penicillin G 2.4 million units IM in a single dose
- Late latent syphilis or latent syphilis of unknown duration – Benzathine penicillin G 7.2 million units total, administered as 3 doses of 2.4 million units IM each at 1-week intervals
- Pregnancy – Treatment appropriate to the stage of syphilis is recommended.
- Following delivery, newborns, were exposed to syphilis in the womb should undergo antibiotic treatment.
Be aware that only benzathine penicillin product (Bicillin L-A) should be used, not benzathine-procaine penicillin (Bicillin C-R). In addition, oral penicillin is never appropriate for the treatment of syphilis.
If the patient arrives late for subsequent doses, clinical experience suggests that an interval of 10-14 days between doses of benzathine penicillin for latent syphilis might be acceptable before restarting the sequence of injections; however, according to pharmacokinetics/pharmacodynamics, an interval of 7-9 days between doses is more optimal. In pregnancy, missed doses are not acceptable. Pregnant patients must repeat the full course of therapy.
In patients with a history of penicillin allergy, desensitization may be necessary in cases of pregnancy, neurosyphilis, congenital syphilis, or tertiary syphilis.
Alternatives to penicillin
Tetracycline, erythromycin, and ceftriaxone have shown antitreponemal activity. A 10- to 14-day trial of ceftriaxone is effective for treating early syphilis. Doxycycline and tetracycline for 28 days have been used for many years and are the only acceptable alternatives to penicillin for the treatment of latent syphilis.
Azithromycin should be used only in areas of low resistance or in early syphilis with close clinical follow-up.
Surgical Care
Surgical care is for treating the complications of tertiary syphilis, like: aortic valve replacement.
Anyone concerned about possible sexually transmitted diseases (STD), need to take medical advice as soon as possible
- Oxford hand Book of medical Dermatology
- ABC Of Dermatology
- Clinical Dermatology
- Roxburgh’s common skin diseases
- Andrew’s Diseases of the skin
STD
TUI - Tibot Urgency Index


Sexually transmitted infections (STI), also referred to as sexually transmitted diseases (STD) and venereal diseases (VD), are infections that are commonly spread by sexual activity, especially vaginal intercourse, anal sex and oral sex. Many times STIs initially do not cause symptoms. This results in a greater risk of passing the disease on to others. Symptoms and signs of disease may include vaginal discharge, penile discharge, ulcers on or around the genitals, and pelvic pain. STIs can be transmitted to an infant before or during childbirth and may result in poor outcomes for the baby. Some STIs may cause problems with the ability to get pregnant.



Syphilis (the Great pox) also known as lues, is an infectious venereal disease caused by the delicate spirochaetal micro-organism Treponema pallidum. The only known host is the human. It is increasing in incidence and is a great mimic. Syphilis is transmissible by sexual contact with infectious lesions, from mother to fetus in uterous, via blood product transfusion, and occasionally through breaks in the skin that come into contact with infectious lesions. If untreated, it progresses through 4 stages: primary, secondary, latent, and tertiary.
Syphilis that remains untreated for a long time can cause major damage to important organs, like the heart and brain. Without treatment, it can lead to disability, and death.
Characteristically, the incubation period is 9–90 days and the first sign is the appearance of the chancre (firm ulcer) at the site of inoculation, usually on the glans penis, prepuce or, less often, on the shaft in men and on the vulva in women. In homosexuals the chancre (firm ulcer) appears around or in the anus. The chancre (firm ulcer) is of variable size (0.5–3 cm in diameter) and has a sloughy and markedly indurated base. Untreated, it heals after 3–8 weeks. The four stages of syphilis are:
- primary
- secondary
- latent
- tertiary
Primary symptoms
One or many painless, firm, and round syphilitic sores called chancres (firm ulcer) are appear. These appear about 18-21 days after exposure.
Chancres (firm ulcer) disappear within 1-4 months, but, without treatment, the disease may progress to the next phase.
In primary syphilis stage also developed regional lymphadenopathy.
Secondary symptoms
Secondary syphilis symptoms include:
- a non-itchy rash/disseminated erythematous rash that is followed by a papulosquamous eruption, that starts on the trunk and spreads to the entire body, including the palms of the hands and soles of the feet and mucous membranes. It may be rough, red, or reddish-brown in color
- Oral(small clustered mouth ulcers), anal, and genital wart-like sores
- muscle aches
- fever
- sire throat
- swollen lymph nodes
- patchy hair loss
- headaches
- weight loss
- fatigue
These symptoms can resolve a few weeks after they appear, or they can return several times over a longer period.
Untreated, secondary syphilis can progress to the latent and late stages.
Latent syphilis
The latent phase can last several years. During this time the body will harbor the disease without symptoms.
After this, tertiary syphilis may develop, or the symptoms may never come back. However, the T. pallidum bacteria remain dormant in the body, and there is always a risk of recurrence.
Late or tertiary syphilis
Tertiary syphilis can occur 10 to 30 years after onset of the infection, normally after a period of latency, where there are no symptoms.
Symptoms include:
- damage to the heart, blood vessels, liver, bones, and joints
- gummas, or soft tissue swellings that occur anywhere on the body
Organ damage means that tertiary syphilis can often be fatal.
Neurosyphilis
Neurosyphilis is a condition where the bacteria have spread to the nervous system. It is often associated with latent and tertiary syphilis, but it can appear at any time after the primary stage.
It may be asymptomatic for a long time, or it can appear gradually.
Symptoms include:
- dementia or altered mental status
- abnormal gait
- numbness in the extremities
- problems with concentration
- confusion
- headache or seizures
- vision problems or vision loss
- weakness
Congenital syphilis
Congenital syphilis is severe and frequently life-threatening. Infection can transfer from a mother to her fetus through the placenta, and also during the birth process.
Without screening and treatment, around 70 percent of women with syphilis will have an adverse outcome in pregnancy.
Adverse outcomes include early fetal death, preterm or low birth weight, neonatal deaths, and infection in infants.
Symptoms in newborns include:
- saddle nose, in which the bridge of the nose is missing
- fever
- difficulty gaining weight
- a rash of the genitals, anus, and mouth
- small blisters on the hands and feet that change to a copper-colored rash and spread to the face, which can be bumpy or flat
- watery nasal fluid
Older infants and young children may experience:
- Hutchinson teeth, or abnormal, peg-shaped teeth
- bone pain
- vision loss
- hearing loss
- joint swelling
- saber shins, a bone problem in the lower legs
- scarring of the skin around the genitals, anus, and mouth
- gray patches around the outer vagina and anus
Infection with the causative organism, Treponema pallidum, may be congenital, acquired through transfusion with contaminated blood, or by accidental inoculation. The most important route, however, is through sexual contact (during oral, anal, or vaginal sexual activity) with an infected partner. Rarely, it can be passed on through kissing.
It can’t be transmitted by sharing a toilet with another person, wearing another person’s clothing, or using another person’s eating utensils.
It can also be passed from mother to a fetus during pregnancy, or to an infant during delivery. This is called congenital syphilis.
Antibiotic Therapy: Penicillin
Penicillin was established as an effective treatment for syphilis. Penicillin is the preferred drug for treating all stages of syphilis. Penicillin is the only recommended therapy for neurosyphilis, congenital syphilis, or syphilis during pregnancy. Rarely, T pallidum has been found to persist following adequate penicillin therapy; however, there is no indication that the organism has acquired resistance to penicillin.
The following regimens are recommended for penicillin treatment:
- Primary or secondary syphilis – Benzathine penicillin G 2.4 million units intramuscularly (IM) in a single dose
- Early latent syphilis – Benzathine penicillin G 2.4 million units IM in a single dose
- Late latent syphilis or latent syphilis of unknown duration – Benzathine penicillin G 7.2 million units total, administered as 3 doses of 2.4 million units IM each at 1-week intervals
- Pregnancy – Treatment appropriate to the stage of syphilis is recommended.
- Following delivery, newborns, were exposed to syphilis in the womb should undergo antibiotic treatment.
Be aware that only benzathine penicillin product (Bicillin L-A) should be used, not benzathine-procaine penicillin (Bicillin C-R). In addition, oral penicillin is never appropriate for the treatment of syphilis.
If the patient arrives late for subsequent doses, clinical experience suggests that an interval of 10-14 days between doses of benzathine penicillin for latent syphilis might be acceptable before restarting the sequence of injections; however, according to pharmacokinetics/pharmacodynamics, an interval of 7-9 days between doses is more optimal. In pregnancy, missed doses are not acceptable. Pregnant patients must repeat the full course of therapy.
In patients with a history of penicillin allergy, desensitization may be necessary in cases of pregnancy, neurosyphilis, congenital syphilis, or tertiary syphilis.
Alternatives to penicillin
Tetracycline, erythromycin, and ceftriaxone have shown antitreponemal activity. A 10- to 14-day trial of ceftriaxone is effective for treating early syphilis. Doxycycline and tetracycline for 28 days have been used for many years and are the only acceptable alternatives to penicillin for the treatment of latent syphilis.
Azithromycin should be used only in areas of low resistance or in early syphilis with close clinical follow-up.
Surgical Care
Surgical care is for treating the complications of tertiary syphilis, like: aortic valve replacement.
Anyone concerned about possible sexually transmitted diseases (STD), need to take medical advice as soon as possible
- Oxford hand Book of medical Dermatology
- ABC Of Dermatology
- Clinical Dermatology
- Roxburgh’s common skin diseases
- Andrew’s Diseases of the skin




