Types Of Blistering Skin Conditions: How to Recognize & Treat Them
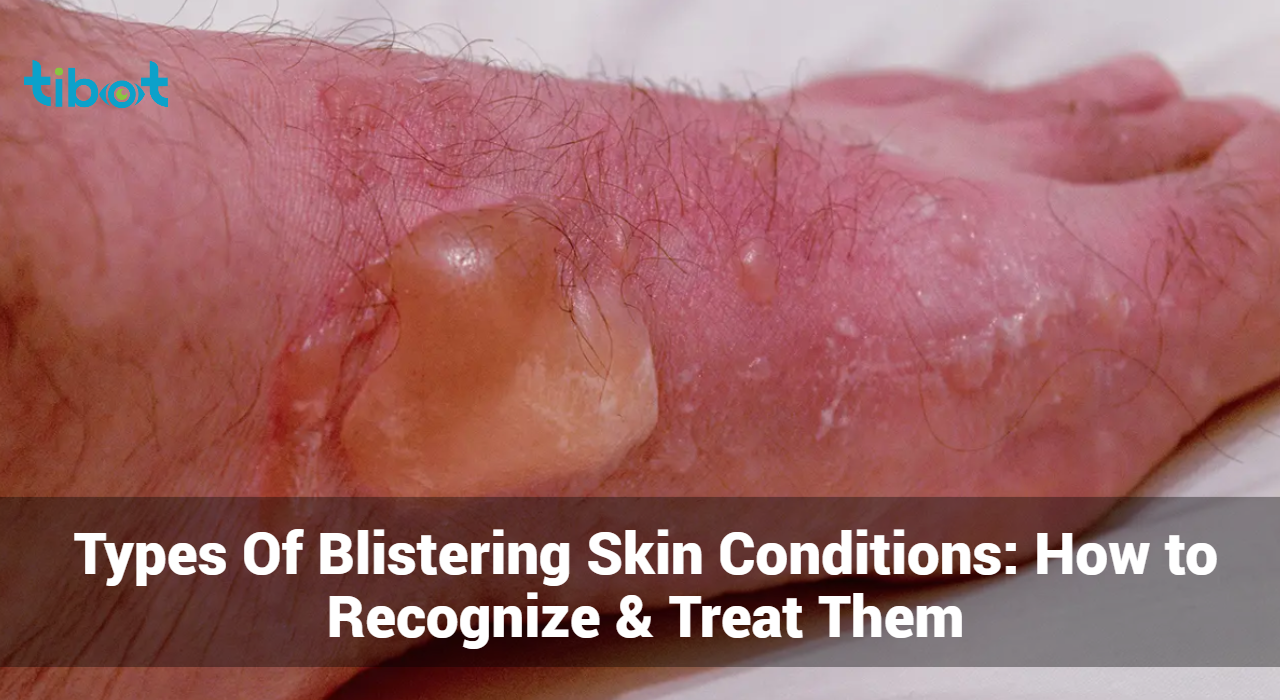
Blistering skin conditions can be both painful and distressing, affecting the skin’s appearance and function. This comprehensive guide will delve into various types of blistering skin conditions, how to recognize them, and effective treatment options. By understanding these conditions, you can better manage symptoms and seek appropriate medical care.
What Are Blistering Skin Conditions?
Blistering skin conditions are a group of disorders characterized by the formation of blisters, which are fluid-filled sacs on the skin. These blisters can vary in size and severity, causing discomfort, pain, and potential complications if not properly managed.
Blisters are fluid-filled sacs that form on the skin due to various factors such as friction, infection, autoimmune responses, or genetic mutations. They can be painful, itchy, and lead to complications if not properly treated.
Common Types of Blistering Skin Conditions
- Pemphigus Vulgaris: Pemphigus vulgaris is an autoimmune disorder where the immune system attacks healthy skin cells, leading to blisters on the skin and mucous membranes.
Symptoms:
- Painful blisters that burst easily
- Open sores on the skin and mouth
- Raw, sensitive skin
Treatment:
- Corticosteroids to reduce inflammation
- Immunosuppressive drugs to decrease immune system activity
- Antibiotics to prevent infections
- Bullous Pemphigoid: Bullous pemphigoid is another autoimmune blistering disorder, primarily affecting older adults. It causes large, fluid-filled blisters, typically on areas prone to flexing.
Symptoms:
- Large blisters that don’t easily burst
- Red, itchy skin around the blisters
- Possible blisters in the mouth
Treatment:
- Corticosteroids to control inflammation
- Immunosuppressive medications
- Antibiotics to manage secondary infections
- Dermatitis Herpetiformis: Dermatitis herpetiformis is a chronic blistering condition linked to gluten sensitivity (celiac disease). It causes itchy, blistering skin lesions.
Symptoms:
- Clusters of itchy, red bumps and blisters
- Burning sensation before blisters appear
- Blisters commonly on elbows, knees, buttocks, and back
Treatment:
- Gluten-free diet to control symptoms
- Dapsone, an antibiotic, to reduce inflammation and itching
- Regular monitoring and blood tests
- Epidermolysis Bullosa (EB): Epidermolysis bullosa is a group of genetic disorders that cause fragile skin, leading to blisters and sores from minor trauma or friction.
Symptoms:
- Blisters and sores from minor injury or friction
- Fragile skin that tears easily
- Scarring and deformities in severe cases
Treatment:
- Wound care to prevent infection
- Pain management
- Nutritional support and physical therapy
- Linear IgA Dermatosis: Linear IgA dermatosis is a rare autoimmune condition that causes blistering and a rash, often in a linear pattern.
Symptoms:
- Itchy, blistering rash
- Blisters often in a line or cluster
- Possible involvement of mucous membranes
Treatment:
- Dapsone to reduce blistering and itching
- Corticosteroids for inflammation control
- Antibiotics for secondary infections
- Physical Examination: Blistering skin conditions are often diagnosed through a physical examination by a dermatologist. The appearance, location, and pattern of blisters can provide important diagnostic clues.
- Skin Biopsy: A skin biopsy involves taking a small sample of affected skin for laboratory analysis. This can help confirm the diagnosis and identify the specific type of blistering condition.
- Blood Tests: Blood tests can detect antibodies associated with autoimmune blistering conditions, helping to pinpoint the exact disorder.
- Genetic Testing: For genetic conditions like epidermolysis bullosa, genetic testing can identify mutations responsible for the disease.
- Direct Immunofluorescence: This test involves examining the skin sample under a microscope to detect specific antibodies that are characteristic of autoimmune blistering diseases.
Treatment Options for Blistering Skin Conditions
Medications
- Corticosteroids: These anti-inflammatory drugs are commonly used to reduce swelling and pain associated with blistering conditions.
- Immunosuppressants: Drugs like azathioprine and mycophenolate mofetil can help manage autoimmune blistering disorders by suppressing the immune system.
- Antibiotics: Used to prevent or treat secondary bacterial infections that can occur in open sores and blisters.
- Dapsone: An antibiotic that is particularly effective in treating dermatitis herpetiformis and linear IgA dermatosis.
Lifestyle and Home Remedies
- Wound Care: Proper wound care is essential to prevent infections and promote healing. This includes cleaning, dressing, and protecting blisters and sores.
- Dietary Changes: For conditions like dermatitis herpetiformis, adhering to a strict gluten-free diet can significantly reduce symptoms.
- Avoiding Triggers: Identifying and avoiding triggers, such as certain foods or environmental factors, can help manage symptoms and prevent flare-ups.
Advanced Treatments
- Biologic Therapies: Biologic drugs, such as rituximab, target specific components of the immune system and can be effective in severe cases of autoimmune blistering diseases.
- Physical Therapy: For genetic conditions like epidermolysis bullosa, physical therapy can help maintain mobility and prevent contractures.
Living with Blistering Skin Conditions
Living with blistering skin conditions can be challenging, but with proper care, support, and management strategies, you can maintain a good quality of life. This guide provides practical tips, treatment options, and lifestyle adjustments to help you navigate daily life with a blistering skin condition.
- Emotional Support: Living with a chronic blistering condition can be emotionally challenging. Support groups, counseling, and mental health services can provide valuable emotional support and coping strategies.
- Education and Awareness: Educating yourself and others about your condition can help reduce misunderstandings and improve social interactions. Awareness campaigns can also promote better understanding and support for those living with blistering skin diseases.
- Regular Medical Care: Regular check-ups with a dermatologist and other healthcare providers are crucial for monitoring the condition, managing symptoms, and adjusting treatment plans as needed.
- Physical Therapy: For conditions like epidermolysis bullosa, physical therapy can help maintain mobility, prevent contractures, and improve overall function.
- Friction and Pressure: Wear loose, soft clothing to minimize friction. Use padded dressings on pressure points.
- Stress: Practice stress-reducing techniques such as yoga, meditation, and deep breathing exercises.
- Sun Protection: Use broad-spectrum sunscreen with at least SPF 30 to protect your skin from UV damage, which can worsen blistering conditions.
- Moisturizing: Keep your skin hydrated with non-comedogenic moisturizers. Look for products designed for sensitive skin.
- Gentle Cleansing: Use mild, fragrance-free cleansers to wash your skin. Avoid harsh soaps and scrubbing, which can aggravate blisters and cause further damage.
- Monitor for Infection: Watch for signs of infection, such as increased redness, swelling, warmth, or pus. Seek medical attention if you suspect an infection.
Analyze Skin Diseases
Use our AI chatbot to determine your skin condition
When to Seek Medical Advice
If you notice persistent or severe blisters, especially those that are painful, itchy, or accompanied by other symptoms like fever or fatigue, it’s important to consult a dermatologist. Early diagnosis and treatment can help manage symptoms and prevent complications.
Conclusion
Blistering skin conditions encompass a range of disorders that can significantly impact quality of life. By understanding the causes, recognizing the symptoms, and exploring various treatment options, individuals can better manage these conditions and maintain healthier skin. If you suspect you have a blistering skin condition, it’s essential to seek medical advice for an accurate diagnosis and appropriate treatment plan.





